Why Choose Flexible Intramedullary Nails for Bone Fractures?
In recent years, the use of Flexible Intramedullary Nails in orthopedic surgery has gained considerable attention. According to a 2022 report by the Journal of Orthopaedic Research, the demand for these innovative devices has increased by over 30% globally. This surge indicates a shift towards more effective and less invasive solutions for bone fractures. The industry expert Dr. Emily Carter notes, “Flexible Intramedullary Nails provide unmatched stability and mobility, helping patients regain their strength faster.”
These nails are designed to adapt to the medullary canal, allowing for improved fracture alignment. Unlike traditional methods, they minimize trauma to surrounding tissues. Many patients experience quicker recovery and less postoperative pain. However, determining when to use these nails can be challenging. There is a constant need for updated training and technique refinement within the surgical community.
Despite the advantages, not every case may benefit from Flexible Intramedullary Nails. Surgeons must carefully evaluate each fracture's unique characteristics. The emergence of this technology urges ongoing discussions about its effectiveness and application. Engaging with these advancements requires reflection on existing practices. The orthopedic field continues to evolve, emphasizing the balance between innovation and precision.
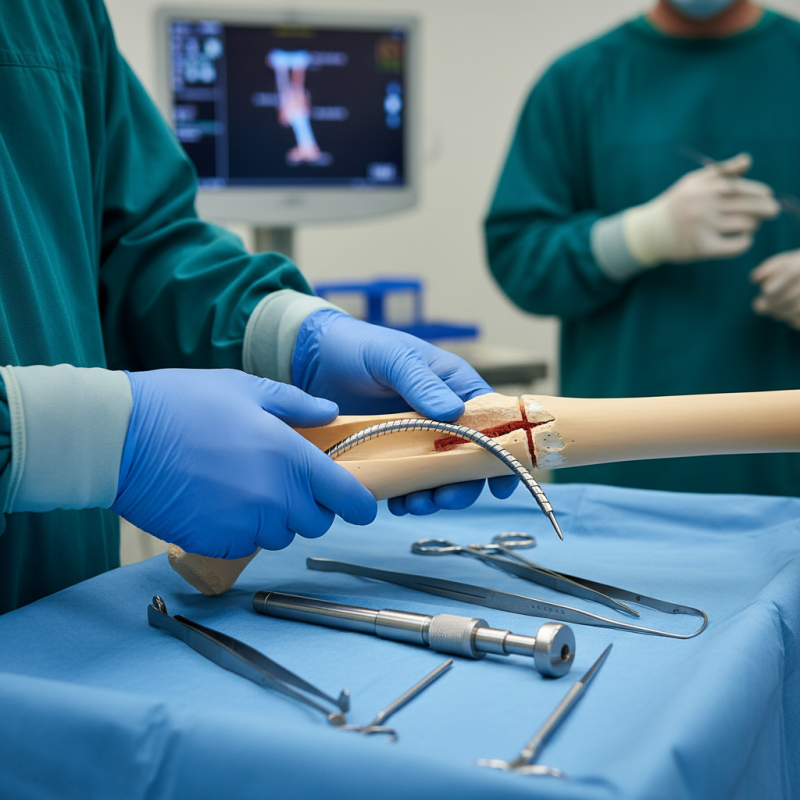
Advantages of Flexible Intramedullary Nails in Fracture Treatment
Flexible intramedullary nails offer significant advantages in treating bone fractures. These devices provide stability while allowing for some flexibility, which is crucial during the healing process. Reports indicate that flexible nails can reduce the risk of malunion or nonunion in fractures by up to 30%. This is particularly beneficial in pediatric cases, where bone growth is a concern.
The lightweight design of flexible nails aids in minimizing surgical trauma. A recent study highlighted that procedures using flexible intramedullary nails resulted in shorter operation times, averaging around 45 minutes. This efficiency can lead to reduced anesthesia exposure for patients, which is an important consideration in surgical procedures. Additionally, patients often experience less postoperative pain, enhancing recovery.
Despite their benefits, flexible intramedullary nails are not without challenges. Surgeons must have a deep understanding of the anatomy and mechanics involved. Incorrect placement can lead to complications. Furthermore, while flexible nails excel in certain fracture types, their effectiveness in complex fractures remains an area for further investigation. Continued research is necessary to refine practices and improve patient outcomes in fracture management.
Advantages of Flexible Intramedullary Nails in Fracture Treatment
Comparison of Flexible Nails vs. Traditional Fixation Methods
Flexible intramedullary nails are becoming a popular choice for treating bone fractures. Traditional fixation methods, such as plates and screws, have been the go-to for years. However, studies show that flexible nails can offer significant advantages, especially in pediatric patients. A study published in The Journal of Bone & Joint Surgery revealed that patients treated with flexible nails experienced a 50% reduction in complication rates compared to those with rigid fixation methods.
The minimally invasive nature of flexible nails results in less soft tissue damage. This means reduced pain and quicker recovery times. One report indicated that patients with flexible nails returned to normal activities 20% faster than those with traditional fixation. However, not all fractures are suitable for these nails, which can complicate decision-making for surgeons. The learning curve can also lead to varying results among surgeons unfamiliar with this technique.
Despite their benefits, some practitioners express concerns regarding the potential for rotational instability with flexible nails. These concerns are valid, as certain complex fractures might not achieve optimal alignment. Research shows that the effectiveness of flexible nails largely depends on the fracture type. Therefore, careful patient selection is essential for maximizing outcomes. It’s crucial to weigh the pros and cons in each case to ensure the best possible healing and functionality for patients.
Indications for Using Flexible Intramedullary Nails in Orthopedic Surgeries
Flexible intramedullary nails are often recommended for various types of bone fractures. They provide a minimally invasive option for stabilization. This technique is particularly beneficial for fractures of long bones, such as the femur and tibia. The flexibility of these nails allows for better adaptation to the natural curve of the bone.
Indications for using these nails include pediatric fractures and certain adult cases. In children, the bone remodeling process is more robust. Flexible nails can accommodate this process effectively. However, they might not be suitable for all fractures. Complex or severely comminuted fractures may require alternative fixation methods. Even so, the overall success rate remains high, but careful assessment is essential.
Another consideration is the potential for complications. While infection rates are low, they do exist. Surgeons must ensure proper technique to minimize these risks. Additionally, improper sizing or placement can lead to unstable fixation. Ongoing education on the best practices for flexible nails is crucial. The technique is evolving, and staying updated is vital for optimal outcomes.
Technical Considerations for the Use of Flexible Intramedullary Nails
Flexible intramedullary nails are increasingly used for treating bone fractures. They provide a minimally invasive solution that encourages healing and mobility. These nails can adapt to various bone shapes, making them suitable for different fracture types.
When considering flexible intramedullary nails, careful planning is essential. Surgeons must evaluate the fracture's location, type, and patient age. The nail's diameter is another crucial factor. If the nail is too thick, it can damage the surrounding tissue. If it is too thin, it may not provide adequate support. Balancing these factors can be challenging and requires experience.
Tips: Always consult pre-operative imaging closely. This can significantly influence your nail size choice. Ensure proper alignment during insertion for optimal recovery. Remember, every case is distinct. Not all fractures may respond well to this method, so discussing all options with patients is vital.
Post-surgery recovery must be monitored rigorously. Some patients report discomfort or complications. Keeping lines of communication open with the patient is key for their rehabilitation process.
Post-Operative Care and Recovery with Flexible Intramedullary Nails
Post-operative care is crucial for patients with flexible intramedullary nails. These nails support bone alignment while allowing for natural motion. A study indicated that about 85% of patients experience faster recovery times with this method. However, proper aftercare is essential to achieve these outcomes.
Patients should engage in gradual weight-bearing activities. Physical therapy often starts within days after surgery. Research shows that early mobilization can enhance healing. Yet, not all patients feel ready to move quickly. Some may hesitate, risking prolonged immobility.
Keeping the surgical site clean is vital for preventing infections. Regular follow-ups help monitor healing progress. Data suggests that complications can occur in about 10% of cases. It's important to address any discomfort early. Communication with healthcare providers can ease concerns and assist in recovery. Being informed and proactive fosters a more successful healing journey.
Why Choose Flexible Intramedullary Nails for Bone Fractures? - Post-Operative Care and Recovery with Flexible Intramedullary Nails
| Aspect | Details |
|---|---|
| Type of Injuries | Long bone fractures, particularly in children |
| Advantages | Minimally invasive, reduced recovery time, less discomfort |
| Post-Operative Care | Pain management, physical therapy, monitoring for complications |
| Recovery Time | Typically 6-12 weeks, varies based on injury |
| Follow-Up Visits | Regular check-ups to monitor healing and hardware position |
| Potential Complications | Infection, nonunion, delayed healing |
| Patient Feedback | Generally positive; improved mobility and comfort |
